Then, at the age of 2, for reaching a more definitive diagnosis of the underlying congenital heart disease, catheteric angiographic studies were performed and right sided aortic arch (RSAA), increased right ventricular (RV) and PA pressures were noticed in these studies. However, after those interventions, clinical symptoms became more severe. Echocardiographic findings revealed severe pulmonary hypertension and large ventricular septal defect (VSD), and due to the severity of pulmonary stenosis (PS), he underwent VSD repair and pulmonary artery (PA) banding operation. Long term examination of his disorder was started from the age of one month by echocardiography. Moreover, all reported cases are type B according to a mirror image of the left-sided arch classification ( 5).Ī 4- year old boy with a history of poor feeding, dyspnea and irritability while feeding that started since infancy was referred to our center. In contrast to the left aortic arch, association of the right-sided aortic arch with aortic arch interruption is extremely rare. 
Tetralogy of Fallot and truncus arteriosus have the most common association with right-sided aortic arch. Right-sided aortic arch is such a rare condition that the prevalence in autopsy and radiographic studies is approximately 0.1% and it is even less common in the setting of normal cardiac situs and almost always has conjunction with other congenital cardiovascular anomalies. Isolated subclavian artery that arises from the ductus arteriosus (sub-type 3) Aberrant subclavian artery (sub-type 2) among which 84% were classified as type B, 13% as type A, and only 3% as type C ( 4).īased on the status of the subclavian artery, each type could be divided into 3 subtypes: In a study, 95 cases of IAA were reviewed by Schreiber et al. In this type, the defect is the most proximal form, occurring between the innominate and left common carotid arteries ( 3). Type C is a very rare type, occurring in less than 5% of IAA cases. This type is an interruption of the aortic arch just distal to the left subclavian artery. Type A is the second most common type and makes up approximately one third of IAA cases. Type B is the most common type (comprising approximately two thirds of all cases) and the defect occurs between the left common carotid and left subclavian arteries. There are three main types of IAA (A, B, and C), which were defined in 1959 according to the anatomical site of the aortic interruption ( 2). Interrupted aortic arch (IAA) is a rare condition that is defined as a lack of luminal continuity between the ascending and descending portions of the Aorta ( 1). 
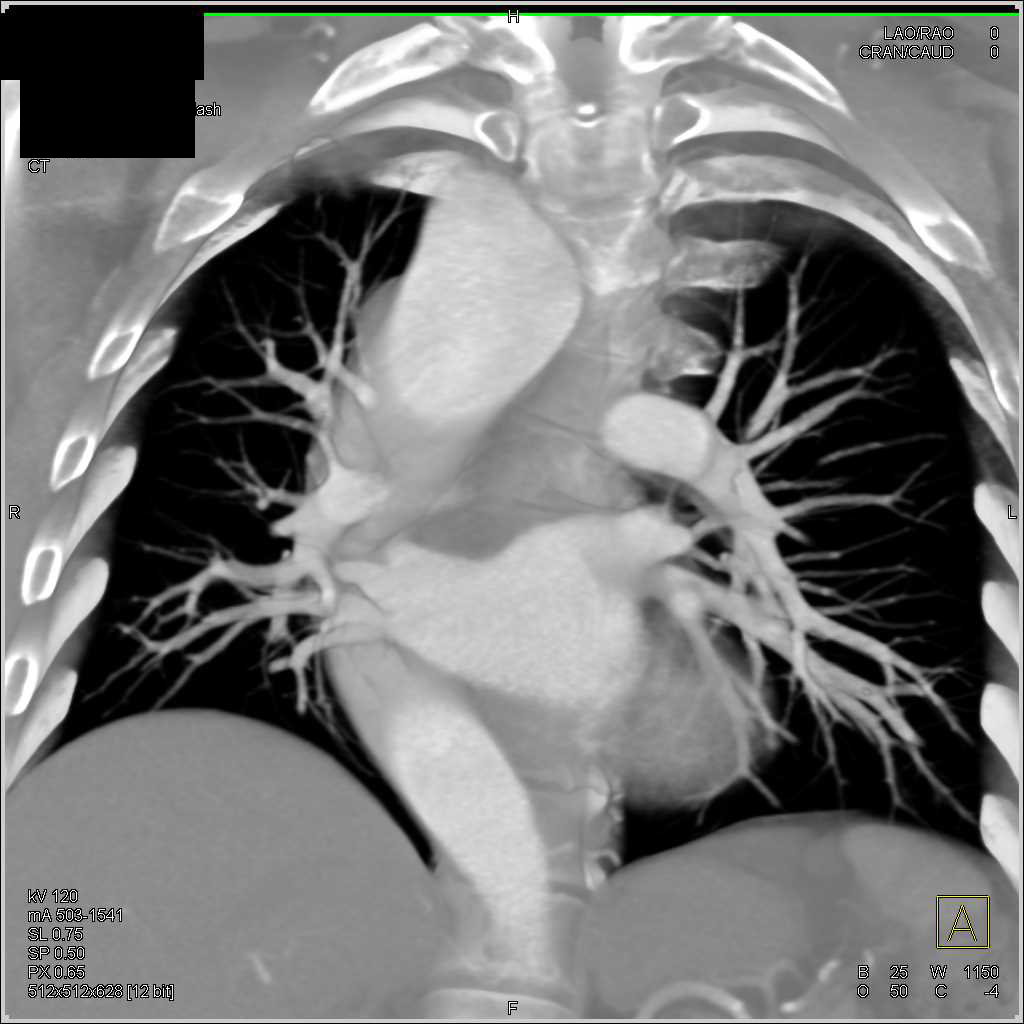
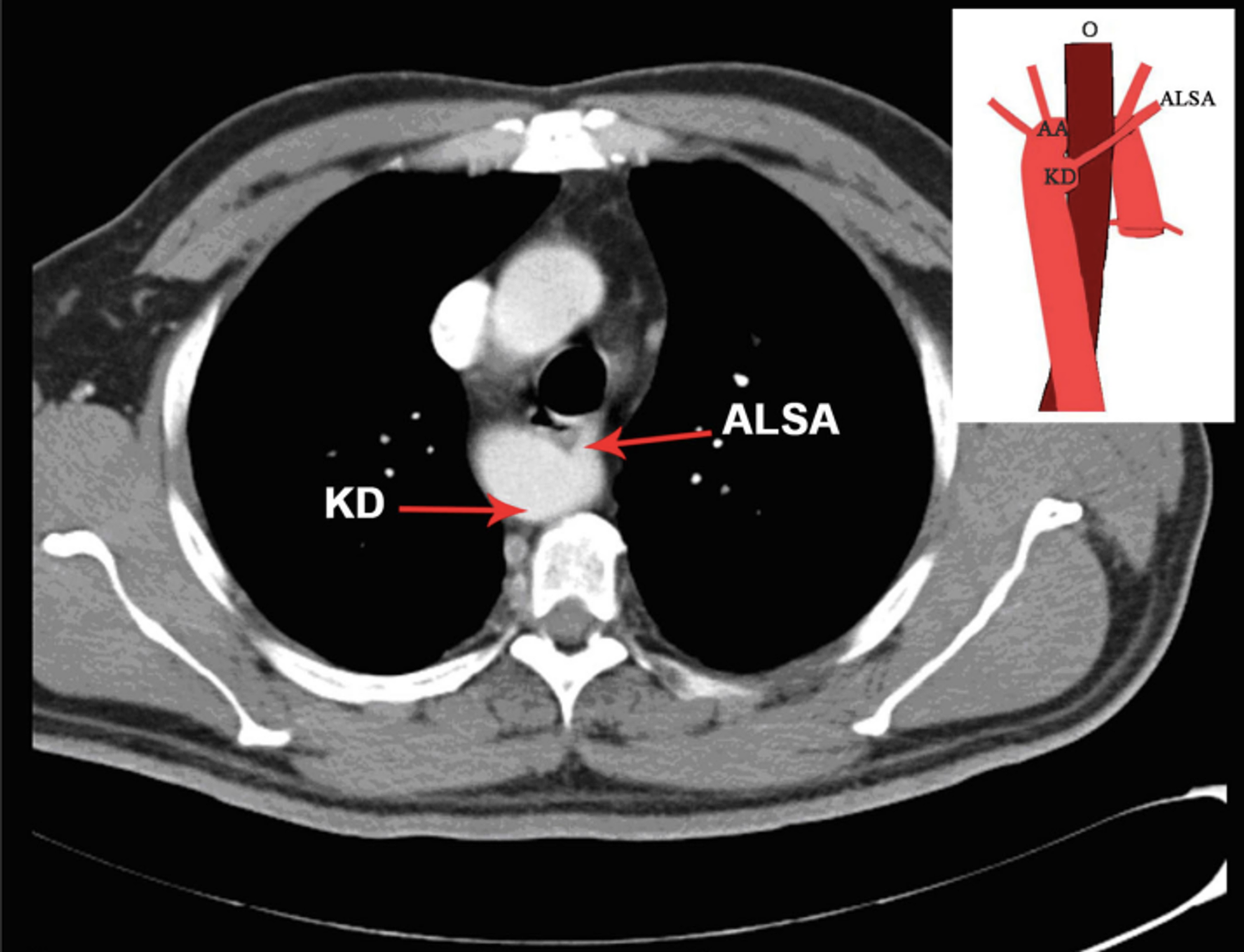
What makes this case report more important is that the authors believe that diagnostic methods in developed countries are able to diagnose this congenital heart disease sooner in neonatal or even in prenatal periods, resulting in a lower incidence of presentation of similar cases in childhood.Ĭardiac Imaging CT-Angiography Pediatrics 1. The symptoms intensified after repairing the patient’s ventricular septal defect (VSD) however, definite diagnosis was obtained by CT angiography. Explanation of this case could be helpful and attractive since echocardiographic and angiographic findings were not definitive enough for final diagnosis of this case. The reason why our case is type C could be explained from an embryologic point of view. Interestingly, almost all types of right sided aortic arch interruptions reported so far were of type B. The computed tomography (CT) angiographic findings revealed type C aortic arch interruption with right sided aortic arch which is a very rare condition and only one similar case has been previously reported in the literature. The patient was referred to our radiographic center and preceeded to undergo CT angiography with multislice spiral thin section scans plus maximum intensity projection (MIP), multiplanar reconstruction (MPR) and volume rendering techniques. Although in all those evaluations, right sided aortic arch (RSAA) and increased right ventricle (RV) and pulmonary artery (PA) pressures were noticed, the definite diagnosis was not reached at that occasion. Long-term examination of the disorder was started by echocardiography since he was one-month old and was performed when he was 2 years old. A 4- year old boy with a history of poor feeding, dyspnea and irritability while feeding that started since infancy, was referred to our center.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
